Natural Approaches to PCOS: Managing a Common Hormonal Imbalance
Polycystic Ovary Syndrome (PCOS) is one of the most common endocrine disorders among women of reproductive age, affecting an estimated 6% to 12% of the female population. This hormonal imbalance can impact both physical and emotional health. In this article, we explore what PCOS is, its causes, symptoms, diagnosis, and above all — natural strategies to support those living with it.
What Is Polycystic Ovary Syndrome (PCOS)?
PCOS is a hormonal condition characterized by excessive androgen production (male hormones) and irregular or absent ovulation. This can lead to irregular periods, infertility, weight gain, and in some cases, ovarian cysts. However, not all women with PCOS have cysts — diagnosis should be based on a combination of symptoms and clinical findings.
Common Symptoms of PCOS
•Irregular menstrual cycles:
Periods may be infrequent, unpredictable, or even absent. This is due to less frequent or absent ovulation, which regulates the menstrual cycle.
•Hirsutism:
Excess androgens can cause the growth of thick, dark hair on areas such as the face, chest, abdomen, or back.
•Weight gain and obesity:
Many women with PCOS struggle with weight, especially around the abdomen, due to insulin resistance.
•Persistent acne:
Hormonal imbalance may lead to acne breakouts on the face, chest, and back.
•Hair thinning:
Some women experience hair thinning or male-pattern baldness.
•Infertility:
Difficulty conceiving is common due to irregular or absent ovulation.
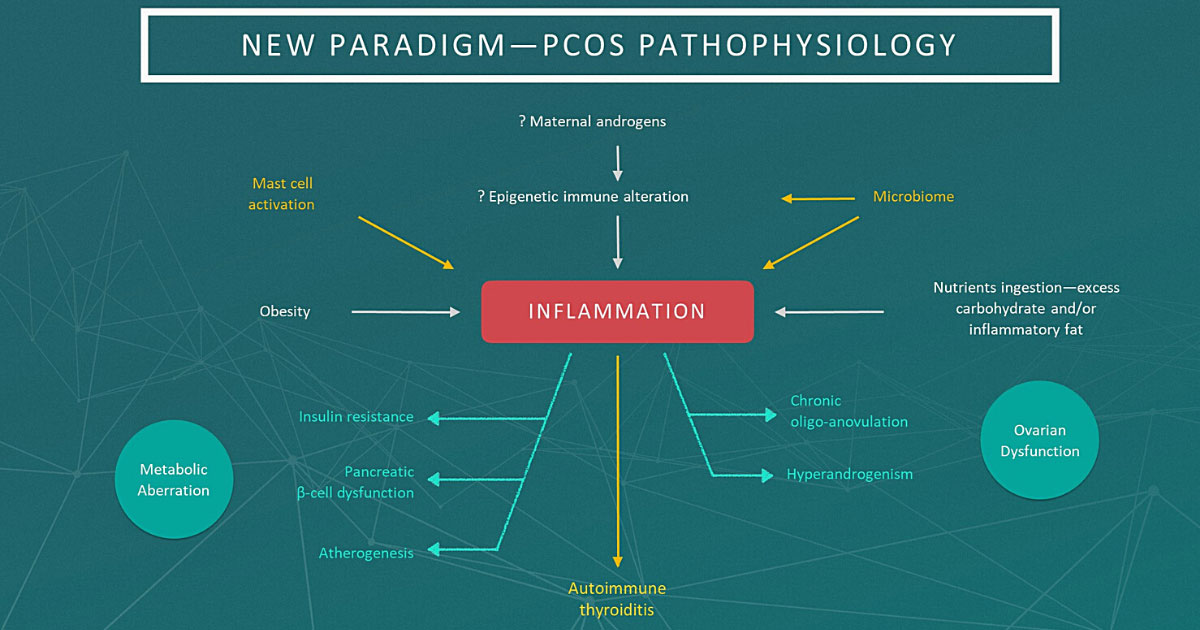
What Causes PCOS?
The exact cause of PCOS is not fully understood, but it is associated with several factors:
•Genetics: Women with a family history of PCOS are more likely to develop it.
•Insulin resistance: The body struggles to process insulin, leading to increased androgen levels.
•Chronic inflammation: Excess inflammation in the body may contribute to hormonal imbalance.
Diagnosing PCOS
PCOS diagnosis requires a multidimensional approach:
1. Detailed medical history: The doctor reviews symptoms, family and menstrual history.
2. Physical examination: Evaluates abnormal hair growth, fat distribution, and other visible indicators of PCOS.
3. Hormonal tests: Blood tests measure levels of androgens, insulin, and other relevant hormones.
4. Pelvic ultrasound: Allows visualization of the ovaries and identification of cysts.
Natural Strategies for Managing PCOS
1. Balanced Anti-Inflammatory Diet
A healthy diet is crucial for managing PCOS. Recommendations include:
•Eat fiber-rich foods: Oats, legumes, and leafy greens help stabilize blood sugar levels.
•Include healthy fats: Avocados, nuts, and olive oil improve insulin sensitivity.
•Avoid processed foods and refined sugars: These reduce inflammation and support hormonal balance.
2. Regular Exercise
Physical activity helps manage weight, improves insulin resistance, and lowers androgen levels. A mix of cardio, strength training, and yoga is ideal.
3. Stress Management
Chronic stress can worsen hormonal imbalances. Mindfulness, meditation, and yoga are effective tools to reduce cortisol (the stress hormone).
4. Nutritional Supplementation
•Inositol: Improves insulin resistance and promotes regular ovulation.
•Vitamin D: Deficiencies are common in women with PCOS; supplementation may help improve symptoms.
•Omega-3s: Essential fatty acids that reduce inflammation and support hormone balance.
Complementary Medical Treatments
In some cases, lifestyle changes need to be supported with medical treatment, such as:
•Oral contraceptives: To regulate menstrual cycles and reduce androgen levels.
•Metformin: Improves insulin sensitivity and may promote ovulation.
•Fertility treatments: Such as clomiphene citrate for women trying to conceive.
The Importance of a Personalized Approach
Every woman is unique, so PCOS management must be personalized. At healthbeyondprotocol.com, Dr. Agnieszka Bil offers a holistic approach that combines conventional medicine with natural strategies to help each patient restore hormonal balance and improve quality of life.
Conclusion
PCOS is a complex condition affecting many aspects of health, but with the right approach, symptoms can be managed and long-term complications prevented. If you suspect you may have PCOS, seek professional guidance. Dr. Agnieszka Bil is here to support your journey toward optimal health.
For more information or to book a session, visit healthbeyondprotocol.com.
Endnotes:
1. Rotterdam ESHRE/ASRM-Sponsored PCOS Consensus Workshop Group. (2004). Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome. Fertility and Sterility, 81(1), 19–25.
• This reference outlines internationally agreed diagnostic criteria for PCOS.
2. Moran, L. J., et al. (2011). Lifestyle changes in women with polycystic ovary syndrome. Cochrane Database of Systematic Reviews, (7), CD007506.
• Provides evidence on the effectiveness of lifestyle changes for managing PCOS.
3. Legro, R. S., et al. (2013). Diagnosis and treatment of polycystic ovary syndrome: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab, 98(12), 4565–4592.
• Offers medical treatment options and recommendations for PCOS.
4. Nestler, J. E., et al. (1998). Role of inositol in ovulation induction in polycystic ovary syndrome. New England Journal of Medicine, 338(26), 1876–1880.
• Research on the benefits of inositol for PCOS patients.
5. Holick, M. F. (2007). Vitamin D deficiency. New England Journal of Medicine, 357(3), 266–281.
• Highlights the importance of vitamin D, including in women with PCOS.
6. Omega-3 in Polycystic Ovary Syndrome Study Group. (2012). Effects of omega-3 fatty acids on insulin resistance and androgen levels in women with PCOS. Am J Clin Nutr, 95(3), 735–741.
• Shows how omega-3s help improve insulin resistance and hormonal balance.
7. Teede, H. J., et al. (2018). International evidence-based guideline for the assessment and management of polycystic ovary syndrome. Human Reproduction, 33(9), 1602–1618.
• A comprehensive international guideline for diagnosing and treating PCOS.




